登录方式
方式一:
PC端网页:www.rccrc.cn
输入账号密码登录,可将此网址收藏并保存密码方便下次登录
方式二:
手机端网页:www.rccrc.cn
输入账号密码登录,可将此网址添加至手机桌面并保存密码方便下次登录
方式三:
【重症肺言】微信公众号
输入账号密码登录
注:账号具有唯一性,即同一个账号不能在两个地方同时登录。
作者:杨柳婷,施熠炜
一、临床资料
患者,女性,40岁,职工,已婚。主因“间断咳嗽、咳痰半年,加重伴发热2月余”于2020年4月22日入院。
患者半年前因“成人Still病”开始口服激素(醋酸泼尼松片20 mg qd)及环孢素(50 mg bid)治疗,用药期间患者出现咳嗽、咳痰症状,黄白色黏痰,量不多,不易咳出,无胸闷、气短、胸痛、咯血等不适,就诊于北京某医院,完善胸部CT示“双肺多发肿块影及结节影,部分内伴空洞”,该院考虑真菌感染,予口服伏立康唑治疗1周。用药后患者咳嗽、咳痰症状一度缓解。自2020年2月开始,患者咳嗽、咳痰加重,间断出现发热,体温最高可达40℃,伴有畏寒,无寒战、呼吸困难等其他症状,调整激素为早晚各一次(醋酸泼尼松片10 mg/次),但患者体温控制较差,于3月15日(图1)及4月20日(图2)复查胸部CT检查,提示双肺多发肿块影及结节影,部分内伴空洞形成,病灶有增大、增多趋势。为求进一步诊治收入我院。
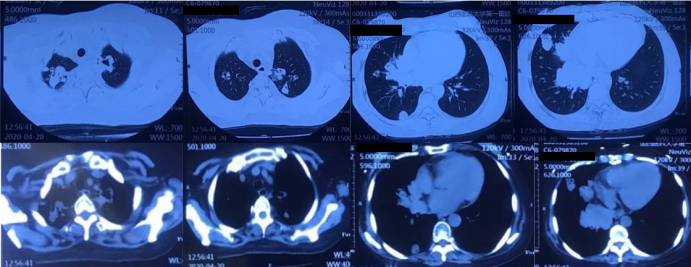
图2 患者胸部CT(2020-04-20)
二、诊疗经过
血气分析(鼻导管吸氧2 L/min):pH 7.51,PaCO2 33 mmHg,PaO2 79.8 mmHg,Na+ 127 mmol/L。
血细胞分析:WBC 10.5×109/L,NEU% 80%,LYM 0.69×109/L。
轻链KAPPA 1.14 g/L,轻链LAMBDA 0.38 g/L,IgA 0.76 g/L,IgG 5.01 g/L,IgM 0.19 g/L。
IL-10 11.63 pg/ml。
镜下所见:气管隆突锐利,左主支气管开口处可见黏性分泌物附着于管壁,充分吸引后见黏膜充血水肿。右主支气管及其右肺中叶可见黏性分泌物附着于管壁,充分吸引后见黏膜充血水肿。余肺各叶段、亚段支气管管腔开口通畅,黏膜轻度充血水肿。于右肺中叶行支气管肺泡灌洗,注入0.9%氯化钠液40 ml,回收淡黄色略浑浊肺泡灌洗液约20 ml。灌洗液分送培养+药敏、找真菌、找结核菌、mNGS、找癌细胞等。
入住风湿免疫科后给予头孢哌酮他唑巴坦2 g q8h、左氧氟沙星0.4 g qd、伏立康唑0.2 g q12h抗感染治疗,患者临床表现无明显变化,遂于4月24日下午转入呼吸与危重症医学科进一步诊治。转入我科后综合评估病情,考虑真菌感染可能性小,特殊病原体感染可能性大,停用伏立康唑,给予口服甲氧苄啶-磺胺甲噁唑(TMP-SMX)2片 q8h。
转入我科第2天晨,患者体温高达39.4℃,脉搏145次/min,呼吸36次/min,血压73/34 mmHg,鼻导管吸氧2 L/min,经皮血氧饱和度90%左右,神志清,精神差,追问患者,其诉前1日因转科忘记服用激素。
复查血细胞分析:NEU% 89.2%,LYM 0.5×109/L,RBC 2.97×1012/L,Hb 90 g/L,HCT 26.9%;IL-6 5000 pg/ml。肝功能:白蛋白26.6 g/L。心肌酶:乳酸脱氢酶537 U/L。超敏CRP 198.47 mg/L。当时立即予静点甲泼尼龙琥珀酸钠40 mg、补液、去甲肾上腺素维持血压,1天后减停血管活性药物。
转入我科1周后,复查胸部CT示肺部病灶较前进一步进展(图3)。患者右小腿皮肤破溃范围扩大至4 cm×7 cm,周围红肿约6 cm×10 cm,肉芽组织不新鲜,有少许分泌物(图4)。此时痰、肺泡灌洗液(BALF)培养及mNGS结果回报均为鼻疽诺卡菌(序列数44783)、金黄色葡萄球菌(序列数187),对TMP-SMX耐药,对美罗培南、利奈唑胺敏感。根据药敏结果换用美罗培南联合利奈唑胺继续抗感染治疗。右小腿皮肤破溃处请中医科会诊后给予中药化腐清创术、去腐生肌膏外用。
图3 患者转入我科1周后复查胸部CT
表1 血细胞分析
调整后治疗效果
三、讨论
参考文献
[1] Tachezy M, Simon P, Ilchmann C, et al. Abscess of adrenal gland caused by disseminated subacute Nocardia farcinica pneumonia. A case report and mini-review of the literature[J]. BMC Infect Dis, 2009, 9:194.
[1] Tachezy M, Simon P, Ilchmann C, et al. Abscess of adrenal gland caused by disseminated subacute Nocardia farcinica pneumonia. A case report and mini-review of the literature[J]. BMC Infect Dis, 2009, 9:194.
[2] Martínez R, Reyes S, Menéndez R. Pulmonary nocardiosis: risk factors, clinical features, diagnosis and prognosis[J]. Curr Opin Pulm Med, 2008, 14(3):219-227.
[3] Takiguchi Y, Ishizaki S, Kobayashi T, et al. Pulmonary Nocardiosis: A Clinical Analysis of 30 Cases[J]. Intern Med, 2017, 56(12):1485-1490.
[4] Kageyama A, Yazawa K, Ishikawa J, et al. Nocardial infections in Japan from 1992 to 2001, including the first report of infection by Nocardia transvalensis[J]. Eur J Epidemiol, 2004, 19(4):383-389.
[5] Torres O H, Domingo P, Pericas R, et al. Infection caused by Nocardia farcinica: case report and review[J]. Eur J Clin Microbiol Infect Dis, 2000, 19(3):205-212.
[6] Mazzaferri F, Cordioli M, Segato E, et al. Nocardia infection over 5 years (2011-2015) in an Italian tertiary care hospital[J]. New Microbiol, 2018, 41(2):136-140.
[7] Minero M V, Marín M, Cercenado E, et al. Nocardiosis at the turn of the century[J]. Medicine (Baltimore), 2009, 88(4): 250-261.
[8] Kiska D L, Hicks K, Pettit D J. Identification of medically relevant Nocardia species with an abbreviated battery of tests[J]. J Clin Microbiol, 2002, 40(4):1346-1351.
[9] Li S, Song X, Zhao Y, et al. Clinical Analysis of Pulmonary Nocardiosis in Patients With Autoimmune Disease[J]. Medicine (Baltimore), 2015, 94(39): e1561.
[10] Kato K, Noguchi S, Naito K, et al. Pulmonary Nocardiosis Caused by Nocardia exalbida in a Patient with Lung Cancer and Radiation Pneumonitis: A Case Report and Literature Review[J]. Intern Med, 2019, 58(11):1605-1611.
[11] Xiao M, Kong F, Sorrell T C, et al. Identification of pathogenic Nocardia species by reverse line blot hybridization targeting the 16S rRNA and 16S-23S rRNA gene spacer regions[J]. J Clin Microbiol, 2010, 48(2):503-511.
[12] Mehrian P, Esfandiari E, Karimi M A, et al. Computed tomography features of pulmonary nocardiosis in immunocompromised and immunocompetent patients[J]. Pol J Radiol, 2015, 80:13-17.
[13] Wang T, Jia Y, Chu B, et al. Nocardiosis in Kidney Disease Patients under Immunosuppressive Therapy: Case Report and Literature Review[J]. Int J Med Sci, 2019, 16(6):838-844.
[14] Kurahara Y, Tachibana K, Tsuyuguchi K, et al. Pulmonary nocardiosis: a clinical analysis of 59 cases[J]. Respir Investig, 2014, 52(3):160-166.
[15] Moylett E H, Pacheco S E, Brown-Elliott B A, et al. Clinical experience with linezolid for the treatment of nocardia infection[J]. Clin Infect Dis, 2003, 36(3):313-318.
[16] Clark N M, Reid G E. Nocardia infections in solid organ transplantation[J]. Am J Transplant, 2013, 13 Suppl 4:83-92.
[17] Roberts S A, Franklin J C, Mijch A, et al. Nocardia infection in heart-lung transplant recipients at Alfred Hospital, Melbourne, Australia, 1989-1998[J]. Clin Infect Dis, 2000, 31(4):968-972.
[18] Smego R A, Jr., Moeller M B, Gallis H A. Trimethoprim-sulfamethoxazole therapy for Nocardia infections[J]. Arch Intern Med, 1983, 143(4): 711-718.
作者简介
杨柳婷
 后可发表评论
后可发表评论




友情链接
联系我们
 公众号
公众号
 客服微信
客服微信